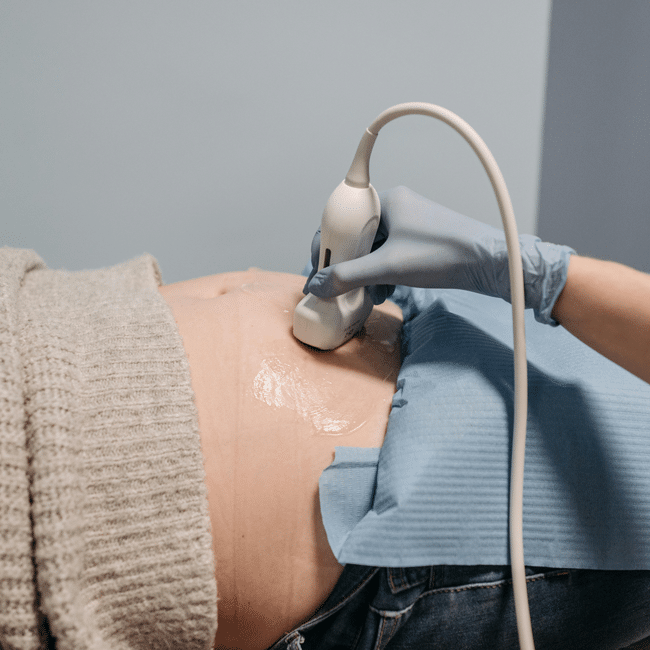
Service for sale: Why privatising public services doesn’t work

Service for sale: Why privatising public services doesn’t work
Opinion + AnalysisHealth + WellbeingBusiness + Leadership
BY Dr Kathryn MacKay 1 OCT 2025
What do the recent Optus 000-incidents, childcare centre abuse allegations, and the Northern Beaches Hospital deaths have in common?
Each of these incidents plausibly resulted from the privatisation of public services, in which the government has systematically disinvested funds and withdrawn oversight.
On the 18th of September, Optus’ 000 service went down for the second time in two years. This time, the outage affected people in Western Australia, and as a result of not being able to get through to the 000 service, it appears that three people have died.
This highlights a more general issue that we see in Australia across a range of public services, including emergency, hospital, and childcare services. The government has sought to privatise important parts of the care economy that are badly suited to generating private profits, leading to moral and practical problems.
Privatisation of public services
Governments in Australia follow economic strategies that can be described as neoliberal. This means that they prefer limited government intervention and favour market solutions to match the value that people are willing to pay with the value that people want to charge for goods and services.
As a result, public goods and services like healthcare, energy, and telecommunications have been gradually sold off in Australia to private companies. This is because, firstly, it’s not considered within the government’s remit to provide them, and secondly, policy makers think the market will provide more efficient solutions for consumers than the government can.
We see then, for example, a proliferation of energy suppliers popping up, offering the most competitive rates they can for consumers against the real cost of energy production. And we see telecommunications companies, like Telstra and Optus, emerging to compete for consumers in the market of cellular and internet services.
So far, so good. In principle, these systems of competition should drive companies to provide the best possible services for the lowest competitive rates, which would mean real advantages for consumers. Indeed, many have argued that governments can’t provide similar advantages for consumers, given that they end up with no competition and no drive for technical improvements.
However, the picture in reality is not so rosy.
Public services: Some things just can’t be privatised
There’s a term in economics called ‘market failure’. This describes a situation where, for a few different possible reasons, the market fails to efficiently respond to supply and demand flows, affecting the nature of public goods and services.
A classic public good has two features: it is non-rival, and non-excludable. A non-rival good is one where one person’s use doesn’t deplete how much of that good is left for others – so we are not rivals because there is enough for everyone. A non-excludable good is one where my use of it doesn’t prevent anyone else from using it either. So, I can’t claim this good because I’m using it right now; it remains open to others to use.
Consider a jumper. This is a rival and excludable good. If I purchase a jumper out of a stock of jumpers, there are fewer jumpers for you and everyone else who wants one. The jumper is a rival good. When I buy the jumper and wear it, no one else can buy it or wear it; it is an excludable good.
Now, consider the 000 service. In theory, if you and I are both facing an emergency, we can both call 000 and get through to an operator. The 000 service is a non-rival, non-excludable good. It is not the sort of thing that anyone can deplete the stock of, nor can anyone exclude anyone else from using it.
Such goods and services present a problem for the market. Private companies have little reason to provide public goods or services, like roads, street lights, 000 services, clean air, or public health care. That’s because these sorts of goods don’t return them much of a profit. There is little or no reason that anyone would pay to use these services when they can’t be excluded from their use and their stock won’t be depleted. Of course, that has not stopped governments from trying to privatise these things anyway, as we see from toll roads, 000, and private care.
Public goods, private incentives
The primary moral problem that arises in the privatisation of public goods and services is two-fold. First, it puts the provision of important goods and services in the hands of companies whose interests directly oppose the nature of the goods to be provided. Second, people are made vulnerable to an unreliable system of private provision of public goods and services.
A private company’s main objective is to make the most possible profit for shareholders. Given that public goods will not make much of a profit, there is little incentive for a private company to give them attention. This means that essential goods and services, like the 000 service, are deprioritised in favour of those other services that will make the company more of a profit.
Further, people become vulnerable to unreliable service providers, as proper oversight and governance undercuts the profit of private companies. Any time a company has to pay for staff re-training, for revision of protocols, or firing and replacing an employee, they make their profits smaller. So, private companies have incentives to cut corners where they can, and oversight, governance, and quality control seem to be the most frequent things to go.
Most of the time, these cut corners go unnoticed. Until, that is, something goes wrong with the service and people get hurt, or worse.
So why does this system continue?
Successive governments have made the decision to privatise goods and services, making their public expenditures smaller and therefore also making it look like they are being more ‘responsible’ with tax revenues. It’s an attractive look for the neoliberal government, which emphasises how small and non-interventionist it is. But is it working for Australians?
It seems like the government’s quest for a smaller bottom line is at odds with the needs of Australian people. The stable provision of a 000 service, safe hospitals with appropriate oversight, and reliable childcare services with proper governance are all essential goods that Australians want, and which private companies consistently seem unable to provide.
It’s a moral – if not economic – imperative that Australian governments reverse course and begin to provide essential goods and services again. The 000 service, the childcare system, and hospitals provide only a few examples of where the government’s involvement in providing public services is very obviously missing. People are getting hurt, and people are dying, for the sake of private profits.
BY Dr Kathryn MacKay
Kathryn is a Senior Lecturer at Sydney Health Ethics, University of Sydney. Her background is in philosophy and bioethics, and her research involves examining issues of human flourishing at the intersection of ethics, feminist theory and political philosophy. Kathryn’s research is mainly focussed on developing a theory of virtue for public health ethics, and on the ethics of public health communication. Her book Public Health Virtue Ethics is forthcoming with Routledge.
Ethics in your inbox.
Get the latest inspiration, intelligence, events & more.
By signing up you agree to our privacy policy
You might be interested in…
Opinion + Analysis
Business + Leadership
Holly Kramer on diversity in hiring
Opinion + Analysis
Business + Leadership
The sponsorship dilemma: How to decide if the money is worth it
Opinion + Analysis
Society + Culture, Health + Wellbeing, Relationships
The price of playtime
Opinion + Analysis
Health + Wellbeing
Democracy is hidden in the data
Women’s pain in pregnancy and beyond is often minimised
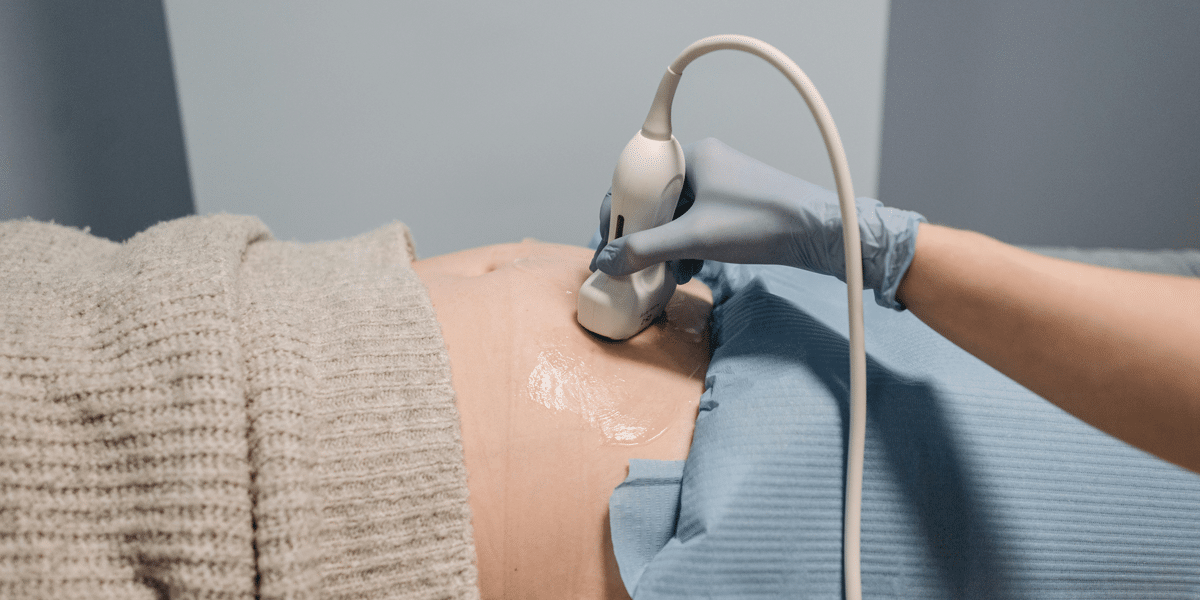
Women’s pain in pregnancy and beyond is often minimised
Opinion + AnalysisHealth + Wellbeing
BY Laura Kotevska 1 OCT 2025
Some recent discussions of pain relief during pregnancy frame the issue of paracetamol use as a maternal-foetal conflict, ignoring science, eroding trust in doctors, dismissing women’s pain, and limiting women’s autonomy. ‘Toughing it out’ is not the answer.
Last week, US president Donald Trump held a press conference announcing the results of his administration’s investigations into the root causes of autism. During the event, he shared several recommendations for the use of acetaminophen (paracetamol) in pregnancy, namely that women should not use it.
Medical experts have criticised the claims as dangerous and poorly informed, and researchers have shown that the recommendations are politicised interpretations of weaker medical studies. In Australia, the Royal Australian and New Zealand College of Obstetricians and Gynaecologists’ recommendations for paracetamol use in pregnancy remain unchanged.
While most expert attention has been paid to debunking the administration’s claims and communicating insights from our best scientific knowledge on the topic, less attention has been given to the tenor of the president’s announcement. How can the ethics of pregnancy help us to understand the rhetorical moves of this speech and how we treat women in pregnancy and beyond?
The ethics of pregnancy care
Trump’s recommendation to avoid paracetamol use in pregnancy is predicated on the assumption that doing so is harmful to the foetus. In this instance, it is recommended that a pregnant woman avoid pain relieving medication on the basis that it may cause autism. Putting aside the fact that there is little evidence of the harmful effects of paracetamol use in pregnancy, the White House press conference framed this issue as a maternal-foetal conflict – an instance of maternal interests (in pain or fever relief) conflicting with the interests of the foetus (of not developing autism). According to the White House, the maternal-foetal conflict should be resolved in favour of the foetus with the recommendation that paracetamol use be avoided in all but the most severe cases. In medicine and maternal decision making, prioritising the foetus is very common, but is hardly a foregone conclusion.
Yet in this instance, and in many other obstetric cases, the central conflict is not between the mother and foetus, but between the mother and others who believe they know better.
Here, the adversary is the White House, and the effect of their remarks is the erosion of trust between the pregnant patient and their physician. This is because the pregnant woman must now contend with information that may contradict her doctor’s advice. Such intervention is “counter-productive relative to the goal of promoting foetal health”, researchers Baylis, Rodgers and Young inform us, since this erosion of trust prevents doctors from providing “the education which would promote the birth of healthier babies”.
Secondly, the maternal-foetal conflict framing ignores the fact that the interests of mother and foetus are inextricably linked. Currently, many health experts are at pains to communicate that paracetamol is a safe for treating fevers and providing pain relief, and that sustained fevers in pregnancy can result in miscarriage, birth malformations and, later, still birth while untreated significant pain can also result in complications. Even in cases where there are certain risks to a foetus, withholding or delaying treatment can potentially lead to increased maternal and foetal morbidity and mortality. The White House’s rhetoric simplifies the often challenging or agonising decisions women and their physicians routinely make during pregnancy.
These examples show that protecting a woman’s health is oftentimes the strongest path to guaranteeing foetal and neonatal outcomes. More than this, recommendations that are laden with unscientific bias erode trust in physicians and limit a woman’s capacity to make informed choices, infringing upon women’s autonomy and potentially risking greater foetal harm.
Toughing it out
It was the experience of giving birth that led the author Anushay Hossain to reflect on the treatment of women’s pain. In The Pain Gap, she writes “Doctors still don’t always believe women when they describe their pain, or they dismiss women’s symptoms as being psychosomatic.” For Hussain, the concept of hysteria is useful to explaining a woman’s experience of the medical system. The common characterisation of women’s pain as hysterical, she writes, shifts blame and judgment onto women. The conversation becomes ‘is your pain real? Is it that bad? Why can’t you cope with it?’
This was the text and subtext of the White House press conference last week. On many occasions in his speech and responses to media outlets, Trump told women to ‘tough it out.’ And if you can’t tough it out? “You know, it’s easy for me to say tough it out, but sometimes in life where a lot of other things, you have to tough it out also. Don’t take Tylenol.” Once again, the blame for pain falls at the feet of women.
Setting aside the aforementioned evidence that women ‘toughing it out’ leads to worse outcomes for their foetuses, telling women to tolerate their pain is not only cruel, but also an example of medical misogyny. Medical misogyny describes the gendered ways patients experience healthcare, often marked by missed diagnoses, delayed treatments, and the dismissal or minimisation of symptoms, including but is not limited to pain. It is startlingly common in Australia with 2 out of 3 women reporting experiences of discrimination in healthcare. For non-white women, the experience is worse.
How should we respond?
To address these widespread issues, governments in Australia and the United Kingdom, among others, have established inquiries into women’s pain and reproductive health. More recently, the Sydney Morning Herald has collected patient testimonies that detail women’s experiences of medical misogyny, bringing about wider awareness of the issue and adding urgency to the call for systemic change.
At a time when many individuals and institutions are working to dismantle the gendered and racial barriers to accessing quality healthcare, dismissing women’s suffering and asking them to ‘tough it out’ reinforces a long history of medical misogyny that leaves women unheard, untreated and unwell.

BY Laura Kotevska
Laura Kotevska is Senior Lecturer in the Office of the Deputy Vice-Chancellor Education and Discipline of Philosophy at the University of Sydney.
Ethics in your inbox.
Get the latest inspiration, intelligence, events & more.
By signing up you agree to our privacy policy
You might be interested in…
Opinion + Analysis
Politics + Human Rights, Health + Wellbeing, Society + Culture
I changed my mind about prisons
Opinion + Analysis
Health + Wellbeing
The virtues of Christmas
Opinion + Analysis
Health + Wellbeing
Democracy is hidden in the data
Opinion + Analysis
Business + Leadership, Health + Wellbeing